In today’s fast-paced world of work, employees expect more than just a paycheck—they expect support, personalization, and simplicity when it comes to their benefits.
But why is employee benefits important? Because when employees don’t understand or trust their benefits, they are less likely to engage with them—directly impacting employee experience, retention, well-being, and organizational cost.
Yet, the reality of benefits administration is often far from ideal: confusing plan options, disjointed communication, and tedious paperwork. HR teams, meanwhile, are juggling complex compliance requirements, vendor integrations, and mountains of employee inquiries.
That’s where Benefits Reimagined steps in.
By embedding artificial intelligence (AI) into benefits delivery, Benefits Reimagined transforms how organizations support their employees—making the entire process smarter, faster, and more human. Let’s explore how AI is reshaping every touchpoint of the employee benefits journey.
The Problem with Traditional Benefits Administration
Let’s face it—benefits administration hasn’t kept up with the expectations of a digital workforce.
Employees often feel overwhelmed when choosing plans, unsure whether they’re making the right financial or medical choices. HR teams struggle with vendor file errors, regulatory pressure, and repetitive support tasks. And employers miss opportunities to build engagement because the system isn’t personalized or predictive.
Key challenges include:
- Disconnected systems and data silos
- Generic, one-size-fits-all communication
- Manual processes for document verification and reconciliation
- Poor visibility into benefits usage and satisfaction
- Lack of predictive insights or personalized support
This isn’t just an administrative problem—it’s a problem of people. Employees who don’t understand or trust their benefits are less likely to engage with them, which directly impacts retention, well-being, and organizational cost.
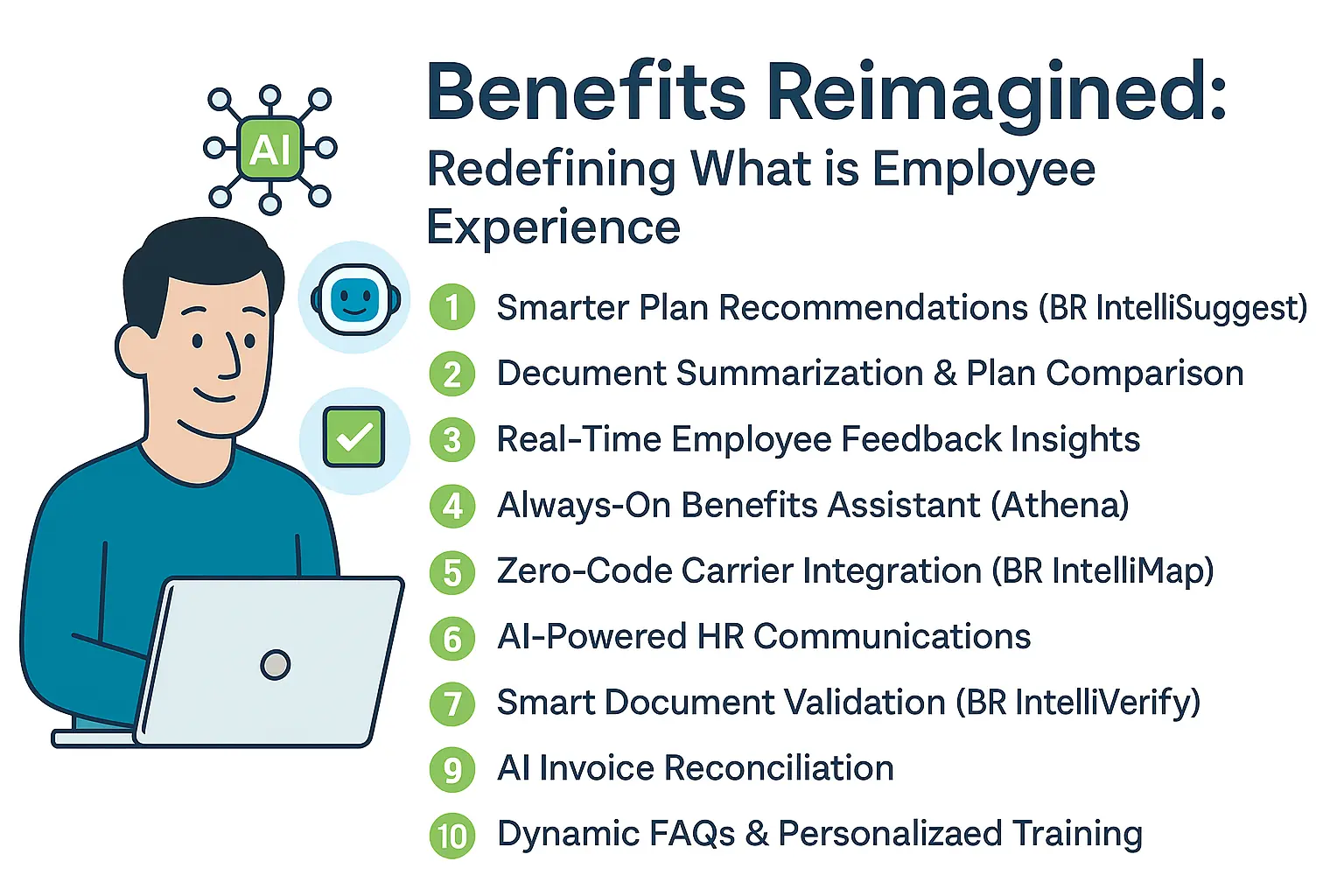
Enter Benefits Reimagined: Redefining What is Employee Experience
At its core, Benefits Reimagined is built around one belief: your benefits should work for you. Not the other way around.
Our AI strategy blends cutting-edge technology with human-centered design to create a more personalized, transparent, and efficient benefits experience. This isn’t about replacing people—it’s about empowering them.
Here’s how:
1. Smarter Plan Recommendations with BR IntelliSuggest
Imagine if Netflix helped you choose a health plan. That’s the idea behind BR IntelliSuggest.
Powered by AI and predictive analytics, this feature looks at an employee’s medical claims, demographic profile, and benefit preferences to recommend the plan that makes the most sense for them. It helps the employee decide what are good employee benefits for that particular employee.
For example:
✅ A healthy young adult might be steered toward a high-deductible plan that maximizes HSA savings.
✅ A parent juggling pediatric visits might get nudged toward a PPO with lower co-pays.
✅ Someone managing a chronic condition could see a comparison showing long-term value in a richer plan, even if the premiums are higher.
No guesswork. Just smart, data-driven guidance.
2. Document Summarization and Side-by-Side Plan Comparison
Let’s be honest—benefits documents are dense. We use AI to cut through the jargon.
With our automated document parsing and summarization engine, employees and HR teams can quickly see how plans compare on key points like premiums, deductibles, coverage limits, and exclusions. It’s like having a benefits expert in your pocket, 24/7.
3. Understanding What is Employee Experience in Real Time
Employee feedback is a goldmine—but only if you can make sense of it.
Using Natural Language Processing (NLP) and sentiment analysis, Benefits Reimagined tracks what employees are saying about their benefits and how they feel about it—whether it’s frustration over high deductibles or appreciation for flexible spending accounts.
With real-time heatmaps and visual reports, HR can spot emerging issues and act before they snowball, helping leaders understand exactly how to improve employee experience.
4. Meet Athena: Your Always-On Benefits Assistant
Athena is our conversational AI chatbot trained specifically for U.S. and Canadian employee benefits.
She doesn’t just answer “What’s my deductible?”—she understands the intent behind questions. Whether employees want to know about their claims, enrollment deadlines, or eligibility, Athena delivers relevant, personalized responses instantly.
Athena also gets smarter over time, using intent analysis and feedback loops to improve continuously. She even integrates with our Communication HUB to guide users to the right place in the app or connect them with human support when needed.
5. Zero-Code Carrier Integration with BR IntelliMap
Integrating with insurance carriers is usually a painful, manual, time-consuming task. Not anymore.
With BR IntelliMap, our AI engine parses carrier companion guides and automatically generates mapping logic for 834 files. This reduces integration time by up to 80%.
No code. No bottlenecks. Just seamless, scalable integration.
6. AI-Powered Writing Assistant for HR Communications
Benefits administrators often spend hours drafting emails, FAQs, and policy updates. Our AI Editor cuts that down dramatically.
From grammar correction to tone adjustment and plagiarism reformation, the Communication HUB’s writing assistant ensures every piece of content is polished, clear, and aligned with your brand voice.
The result? Better communication, faster execution, and higher engagement.
7. BR IntelliVerify: Intelligent Document Validation
Dependent verification is one of the most error-prone and resource-intensive tasks in HR.
BR IntelliVerify uses OCR and AI to automatically extract, validate, and analyze uploaded documents—flagging issues like missing pages, mismatched data, or possible tampering.
Admins get a clean interface to review, approve, or escalate cases, with a full audit trail powered by Elasticsearch.
8. Invoice Reconciliation with AI Accuracy
Carrier invoices can be a black box. With AI, we turn them into a transparent, accurate part of your workflow.
Benefits Reimagined scans, classifies, and extracts data from carrier invoices—then compares them to actual employee records. Discrepancies are flagged and shared in a clear reconciliation report.
No more surprises. No more overpayments.
9. Automated Emails with a Human Touch
Employees often ask the same three questions:
- Am I eligible for this benefit?
- What’s the status of my claim?
- When’s the enrollment deadline?
Our auto-response system drafts intelligent replies using generative AI—and gives HR the ability to review and approve them through a “human-in-the-loop” UI.
It’s a perfect blend of automation and oversight, designed for speed without sacrificing empathy.
10. Dynamic FAQs and Personalized Training
Gone are the days of static PDF guides.
Benefits Reimagined’s AI-powered FAQ and onboarding system learns from employee behavior and HR feedback to generate tailored answers, interactive training modules, and real-time assistance.
Whether it’s a new hire learning about dental coverage or a seasoned employee curious about wellness stipends, the platform adjusts content to their needs and preferences.
Bringing It All Together: The AI-Powered Benefits Employee Experience
Benefits Reimagined isn’t just digitizing processes—it’s rethinking them. By building AI into the foundation of the platform, we’re enabling:
- More informed decision-making
- Reduced administrative overhead
- Greater personalization
- Real-time insights
- Scalable integrations
And above all—a better employee experience
This is the future of benefits. Intelligent, inclusive, and employee-first.
Discover how Benefits Reimagined can transform your workplace today.